
The Physicians' Workforce Projections Committee ended its 30th session after concluding that "as many as 11,136 physicians may be lacking by 2040," yet controversy surrounding a "hasty declaration" continues. Although the group was established to accurately assess the necessary number of medical professionals in the future, it supposedly provided unclear data without sufficient validation, focusing more on meeting the time limit than ensuring accuracy. Several committee members reportedly stated, "This is comparable to a college-level paper" and "It's difficult to view this as genuine statistical analysis."
At the last meeting, the committee focused mainly on deciding which predictive model to use for forecasting future physician demand and availability, instead of improving the models.
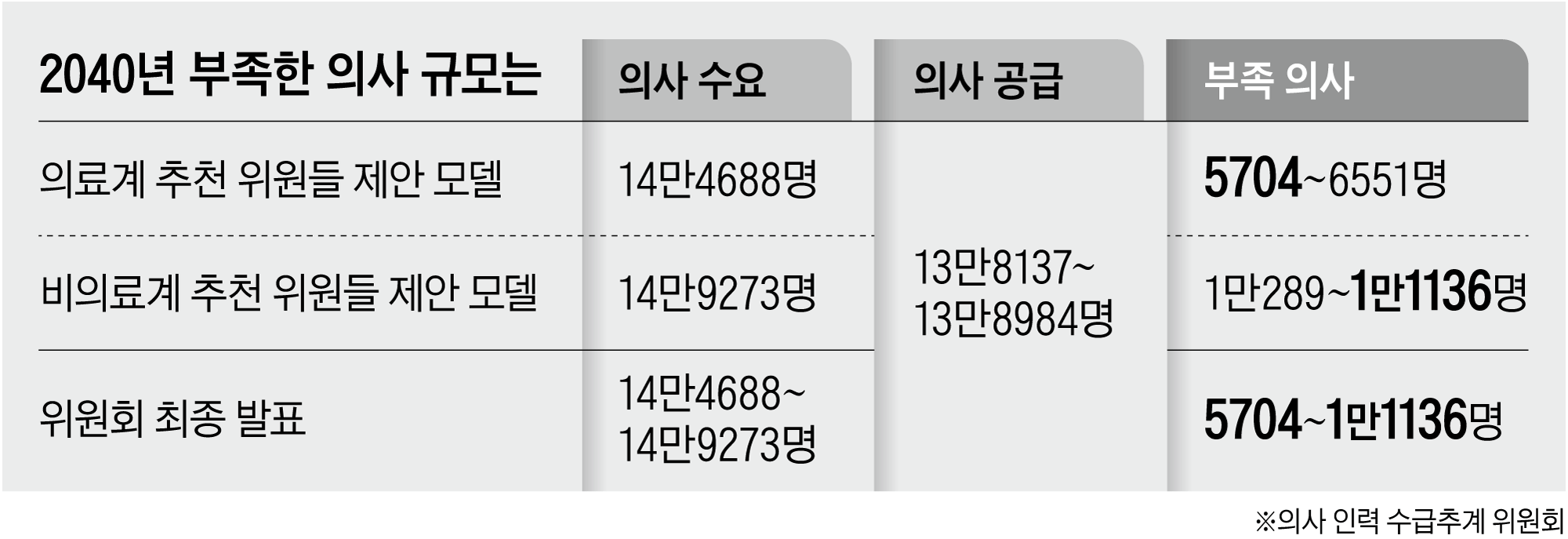
As per a report published by this newspaper on December 31, there was minimal dispute among committee members regarding the total number of physicians expected to be available by 2040. Instead, the debate focused on the method used to calculate the necessary quantity of doctors. During the meeting, three distinct approaches were introduced, each yielding vastly differing estimates for the required physician count. Members from non-healthcare backgrounds mainly endorsed one approach forecasting a demand for 149,273 doctors by 2040. The remaining two methods suggested much lower quantities. Nevertheless, the committee approved all three models, leading to a wide variation in predicted medical professional deficits — ranging between 5,704 and 11,136 by 2040. Earlier, on December 8, the committee reviewed an initial projection indicating a potential shortfall of as many as 18,700 doctors by 2040; however, this estimate dropped by more than 7,000 within approximately three weeks.
This sparked backlash: "I fail to notice how this differs from the Yoon Suk-yeol administration's unilateral methods." Under the Yoon leadership, officials advocated for raising the number of medical students admitted by 2,000, arguing that "there would be a shortage of 15,000 physicians by 2035." A new review conducted by the Board of Audit and Inspection revealed that during the Yoon era, a publicly funded research institute revised an earlier analysis—originally stating that "11,527 doctors would be lacking by 2035"—so it supported the assertion that "physicians were already experiencing shortages." Following a survey showing that "4,786 doctors were missing in regions with limited healthcare access," authorities merged this data with previous estimates (11,527) to determine that "a total of 16,313 doctors will be insufficient by 2035."
A major topic addressed by the committee was determining how to assess future physician needs. This calculation depends on information about the number of hours physicians work annually and daily. Nevertheless, the committee did not have this data and therefore relied on "medical utilization rates" derived from hospital admission figures.
Moreover, it did not adequately consider shifts in productivity resulting from the integration of artificial intelligence or the growing preference among younger physicians for better work-life balance and reduced working hours. The committee referenced an OECD study to suggest a situation in which AI enhances physician efficiency by 6%, yet this percentage was applied across the whole health care industry, rather than specifically to medical professionals. Additionally, it made an assumption—without solid support—that doctors' working days would decline by 5% by 2040. A member of the committee remarked, "They arrived at a 'no effect' outcome by combining claims that AI lessens the demand for doctors and that shorter workdays raise the necessity."
This approach to decision-making differs from situations abroad. For example, Japan distinguishes between demands for clinical and non-clinical physicians and utilizes regional surveys to assess requirements for both inpatients and outpatients. It takes into account the number of doctors required per hospital bed as well as the proportion of doctors relative to outpatient consultations. In the UK, forecasting healthcare staffing needs includes input from medical boards along with the Office of Auditors and Inspectors. Previous studies have examined factors such as initial outpatient appointment rates, increases in emergency department visits, and the share of patients on waitlists who ultimately did not receive treatment.


0 Komentar